Knee
- Anatomy
- Conditions
- Procedures
Knee Anatomy
The knee is a complex joint made up of different structures including bones, tendons, ligaments and muscles. They all work together to maintain normal function and provide stability to the knee during movement.
Having a well-functioning healthy knee is essential for our mobility and ability to participate in various activities. Understanding the anatomy of the knee enhances your ability to discuss and choose the right treatment procedure for knee problems with your doctor.
Bones
The Knee is a hinge joint made up of two bones, the thighbone (femur) and the shinbone (tibia). There are two round knobs at the end of the femur called femoral condyles which articulate with the flat surface of the tibia called the tibial plateau. The tibia plateau on the inside of the leg is called the medial tibial plateau, and on the outside of the leg it is called the lateral tibial plateau.
The two femoral condyles form a groove on the front (anterior) side of the knee called the patellofemoral groove. A small bone called the patella sits in this groove and forms the kneecap. It acts as a shield and protects the knee joint from direct trauma.
A fourth bone called the fibula is the other bone of the lower leg. This forms a small joint with the tibia. This joint has very little movement and is not considered a part of the main joint of the knee.
Articular Cartilage and Menisci
Movement of the bones causes friction between the articulating surfaces. To reduce this friction, all articulating surfaces involved in movement are covered with a white, shiny, slippery layer called articular cartilage. The articulating surface of the femoral condyles, tibial plateaus and the back of the patella are covered with this cartilage. The cartilage provides a smooth surface that facilitates easy movement.
To further reduce friction between the articulating surfaces of the bones, the knee joint is lined by a synovial membrane which produces a thick clear fluid called synovial fluid. This fluid lubricates and nourishes the cartilage and bones inside the joint capsule.
Within the knee joint between the femur and tibia there are two C shaped cartilaginous structures called menisci. Menisci function to provide stability to the knee by spreading the weight of the upper body across the whole surface of the tibial plateau. The menisci help in load bearing by preventing the weight from concentrating onto a small area, which could damage the articular cartilage. The menisci also act as a cushion between the femur and tibia by absorbing the shock produced by activities such as walking, running and jumping.
Ligaments
Ligaments are tough bands of tissue that connect one bone to another bone. The ligaments of the knee function to stabilise the knee joint. There are two important groups of ligaments that hold the bones of the knee joint together, collateral ligaments and the cruciate ligament.
Collateral ligaments: Collateral ligaments are present on either side of the knee. They function to prevent the knee from moving too far during side to side motion. The collateral ligament on the inside is called the medial collateral ligament (MCL) and the collateral ligament on the outside is called the lateral collateral ligament (LCL).
Cruciate ligaments: This group of ligaments, present inside the knee joint, control the back and forth motion of the knee. The Cruciate ligament in the front of the knee is called anterior cruciate ligament or ACL and the cruciate ligament in the back of the knee is called posterior cruciate ligament or PCL.
Muscles
There are two major muscles, the quadriceps and the hamstrings, which enable movement of the knee joint. The quadriceps muscles are in the front of the thigh. When the quadriceps muscles contract, the knee straightens. The hamstrings are in the back of the thigh. When the hamstring muscles contract, the knee bends.
Tendons
Tendons are structures that attach muscles to the bone. The quadriceps muscles of the knee meet just above the patella and attach to it through a tendon called the quadriceps tendon. The patella further attaches to the tibia through a tendon called the patella tendon. The quadriceps muscle, quadriceps tendon and patellar tendon all work together to straighten the knee. Similarly, the hamstring muscles at the back of the leg are attached to the knee joint with the hamstring tendon.
Conditions

Lateral Meniscus Syndrome
The knee joint is formed by the union of two bones, namely the femur (thigh bone) and the tibia (lower leg bone). At the junction of these two bones is a cartilage called the meniscus, which acts as a shock absorber. There are two menisci – the lateral and medial menisci. The lateral meniscus is the outer meniscus of the knee joint and gives a cushioning effect during weight bearing activities. Lateral meniscus syndrome is characterised by an injury caused by the tearing of the cartilage tissue or a rare case of a congenital abnormality called a discoid meniscus, which results in knee pain.


Knee Angular Deformities (Knock legs and Bow legs)
Angular deformities of the knee are common during childhood and usually are variations in the normal growth pattern. Angular deformity of the knee is a part of normal growth and development during early childhood. Physiologic angular deformities vary with age as:
- During first year: Lateral bowing of tibia
- For second year: Bow legs (knees and tibia)
- Between 3-4 years: Knock Knees
Knee Pain
The knee is one of the largest joints in the body, formed by the lower end of the femur, upper end of the tibia and the patella or kneecap. Several ligaments and muscles attach to the bones of the knee joint to maintain normal motion of the joint. Special cartilaginous tissues known as menisci are placed between the two articular ends of the joint. These act as a cushion between the articular surfaces and absorb the shock during movement.
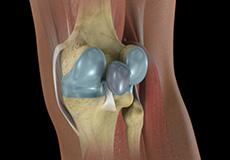
Baker’s Cyst
The knee consists of a fluid called synovial fluid, which reduces friction between the bones of the knee joint while you move your leg. Sometimes this fluid is produced in excess, resulting in its accumulation in the back of your knee. A Baker’s cyst or popliteal cyst is a fluid-filled swelling that develops into a lump behind the knee. This causes stiffness, tightness and pain behind your knee. It is commonly seen in women and people aged over 40 (although it can develop at any age).
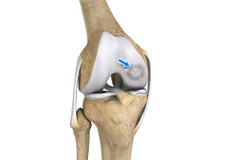
Osteochondritis Dissecans
Osteochondritis dissecans is a joint condition in which a piece of cartilage, along with a thin layer of the bone separates from the end of the bone because of inadequate blood supply. The separated fragments are sometimes called “joint mice”. These fragments may be localised, or may detach and fall into the joint space causing pain and joint instability.
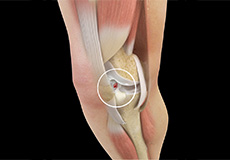
ACL Tears
The anterior cruciate ligament, or ACL, is one of the major ligaments of the knee that is in the middle of the knee and runs from the femur (thighbone) to the tibia (shinbone). It prevents the tibia from sliding out in front of the femur. Together with posterior cruciate ligament (PCL) it provides rotational stability to the knee.
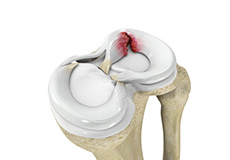
Meniscal Tears
Meniscus tear is the commonest knee injury in athletes, especially those involved in contact sports. A sudden bend or twist in your knee cause the meniscus to tear. This is a traumatic meniscus tear. Elderly people are more prone to degenerative meniscal tears as the cartilage wears out and weakens with age. The two wedge-shape cartilage pieces present between the thighbone and the shinbone are called meniscus. They stabilise the knee joint and act as “shock absorbers”.
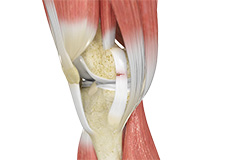
Ligament Injuries
The knee is a complex joint which consists of bone, cartilage, ligaments and tendons that make joint movements easy and at the same time more susceptible to various kinds of injuries.
Knee problems may arise if any of these structures get injured by overuse or suddenly during sports activities. Pain, swelling, and stiffness are the common symptoms of any damage or injury to the knee.
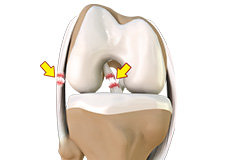
Multiligament Instability
The knee is a complex joint of the body which is vital for movement. The four major ligaments of the knee are anterior cruciate ligament, posterior cruciate ligament, medial collateral ligament and lateral collateral ligament. They play an important role in maintaining the stability of the knee. An injury resulting in tear of one or more ligaments of the knee thus affects knee stability. Such injuries occur because of direct blow to the knee, or a fall from a height, or motor vehicle trauma.
Knee Arthritis
Arthritis is a general term covering numerous conditions where the joint surface or cartilage wears out. The joint surface is covered by a smooth articular surface that allows pain free movement in the joint. This surface can wear out for several reasons; often the definite cause is not known.
Patellar Dislocation/Patellofemoral Dislocation
Patella (kneecap) is a protective bone attached to the quadriceps muscles of the thigh by quadriceps tendon. Patella attaches with the femur bone and forms a patellofemoral joint. Patella is protected by a ligament which secures the kneecap from gliding out and is called as medial patellofemoral ligament (MPFL).
PCL Injuries
Posterior cruciate ligament (PCL), one of four major ligaments of the knee are situated at the back of the knee. It connects the thighbone (femur) to the shinbone (tibia). The PCL limits the backward motion of the shinbone.
PCL injuries are very rare and are difficult to detect than other knee ligament injuries. Cartilage injuries, bone bruises, and ligament injuries often occur in combination with PCL injuries.
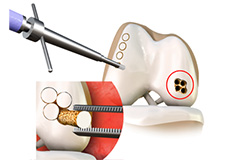
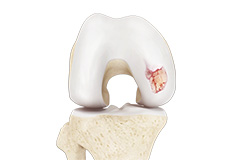
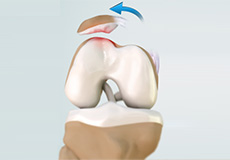
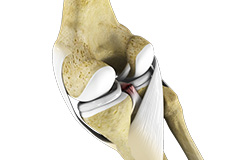
Chondral (Articular Cartilage Defects)
Articular or hyaline cartilage is the tissue lining the surface of the two bones in the knee joint. Cartilage helps the bones move smoothly against each other and can withstand the weight of the body during activities such as running and jumping. Articular cartilage does not have a direct blood supply to it so has less capacity to repair itself. Once the cartilage is torn it will not heal easily and can lead to degeneration of the articular surface, leading to development of osteoarthritis.
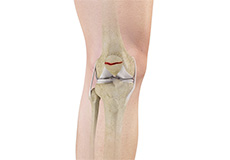
Patella Fracture
The kneecap or patella is the largest sesamoid bone in the body and one of the components of the knee joint, present at the front of the knee. The under surface of the kneecap and the lower end of the femur are coated with articular cartilage, which helps in smooth movement of the knee joint. The kneecap protects the knee and provides attachment to various muscle groups of the thigh and leg. Fracture of kneecap is rare and is more common in adult males.
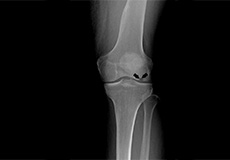
Osteonecrosis of the Knee
Osteonecrosis is a condition in which death of a section of bone occurs because of lack of blood supply to it. It is one of the most common causes of knee pain in older women. Women over the age of 60 years of age are commonly affected, three times more often than men.
Osteonecrosis of the knee is most commonly seen in the femoral condyle, usually on the inner side of the knee (the medial femoral condyle).
Procedures
Surgical Treatment
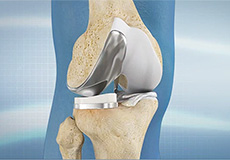
Partial Knee Resurfacing
Partial knee replacement is an alternative to total knee replacement in patients with arthritis on only one side of the knee. Partial knee replacement is a surgical procedure which involves resurfacing and replacement of only the diseased surface of the joint instead of the entire joint.
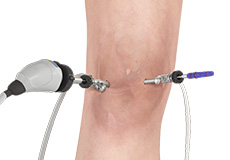
Knee Arthroscopy
Knee arthroscopy is commonly called keyhole surgery or a knee scope. It is an operation which involves looking inside the knee joint using a camera.
Knee arthroscopy is performed as a day case operation, which means that you don’t need to stay overnight. Usually you come in early in the morning and go home early in the afternoon or come in late in the morning and go home early in the evening – depending on whether it is a morning or afternoon list.
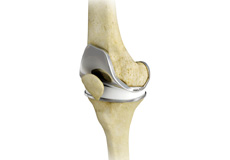
Knee Replacement
You will be admitted to hospital either on the morning of your operation or sometimes the night before. The nursing staff will meet you on your arrival. One of the hospital medical doctors will review you during your stay to monitor your general health (this is most often Dr Adrienne Anderson). The anaesthetist will see you on the day of your operation and go over your medical conditions and discuss the anaesthetic. I will see you on the day of your operation, before the surgery, and draw an arrow on your knee to confirm which side we are operating on and to answer any of your questions.
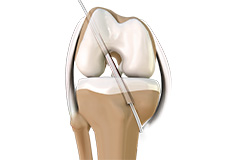
ACL Reconstruction
ACL Injury is a common problem in which one of the main ligaments which keeps your knee stable to walk on is torn. The ACL is a thick fibrous band that sits in the centre of your knee and holds the femur and tibia bones firmly together. It prevents the bones from sliding back and forth too much when you walk and run, and particularly when you change direction quickly.
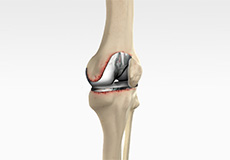
Revision Knee Replacement
Revision knee replacement surgery involves replacing part or all your previous knee prosthesis with a new prosthesis. Although total knee replacement surgery is successful, sometimes the procedure can fail due to various reasons and require a second revision surgery.
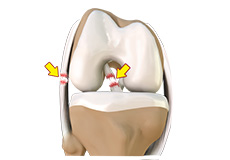
Multi Ligament Reconstruction
The knee is the most complex joint in the body and is formed by the articulation between the thighbone (femur) and the shinbone (tibia). A kneecap is present over the front of the joint to provide extra protection. These bones are held together by four strong rope like structures called ligaments. Two collateral ligaments are present on either side of the knee and control the sideway movements of the knee. The other two ligaments are the anterior and posterior cruciate ligaments, ACL and PCL respectively, which are present in the centre of the knee joint and cross each other to form an “X”. The cruciate ligaments control the back and forth movement of the knee.
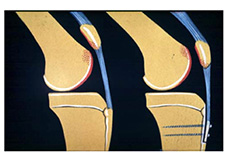
Distal Realignment Procedures
Distal realignment procedures, also known as TTT or tibial tubercle transfer procedures are performed to reposition the kneecap by realigning the tendon under the kneecap to the underlying tibial tubercle. Tibia tubercle is the bony lump on the tibia (bone in the lower leg) below the kneecap. This serves as an attachment point for the patellar ligaments, tendons, and muscles. These procedures are done to prevent patellar subluxation or dislocation.
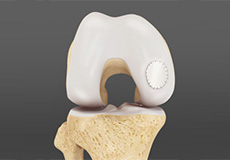
Cartilage Replacement
Cartilage replacement is a surgical procedure performed to replace the worn-out cartilage with the new cartilage. It is usually performed to treat patients with small areas of cartilage damage usually caused by sports or traumatic injuries. It is not indicated for those patients who have advanced arthritis of knee. Articular or hyaline cartilage is the tissue that covers bone surface of the knee which helps in smooth interaction between the two bones in knee joint.
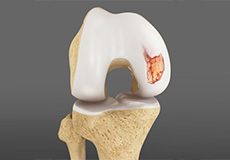
Cartilage Repair and Transplantation
Articular Cartilage is the white tissue lining the end of bones where these bones connect to form joints. Cartilage acts as cushioning material and helps in smooth gliding of bones during movement. An injury to the joint may damage this cartilage which cannot repair on its own. Cartilage can be damaged with increasing age, normal wear and tear, or trauma. Damaged cartilage cannot cushion the joints during movement and the joints may rub over each other causing severe pain and inflammation.

Sports Medicine
Sports injuries occur when playing indoor or outdoor sports or while exercising. They can result from accidents, inadequate training, improper use of protective devices, or insufficient stretching or warm-up exercises. The most common sports injuries are sprains and strains, fractures and dislocations.